Torsemide vs. Lasix: The Diuretic Duel You Didn't Know You Needed
Table of Contents
- Introduction
- Understanding Diuretics
- What Is Lasix?
- What Is Torsemide?
- Onset and Duration: Speed vs. Endurance
- Effectiveness in Heart Failure
- Electrolyte Impact and Safety Profile
- Cost and Availability
- Patient Experiences and Clinical Preferences
- Which One Should You Choose?
Introduction
Diuretics—commonly known as "water pills"—are a cornerstone of treatment for heart failure, hypertension, and fluid retention. While Lasix (furosemide) has long been the poster child of loop diuretics, another contender is stepping into the ring: Torsemide. With improved bioavailability and longer action, Torsemide is being hailed as a potential replacement. But is it truly better? Let’s unpack this diuretic showdown. 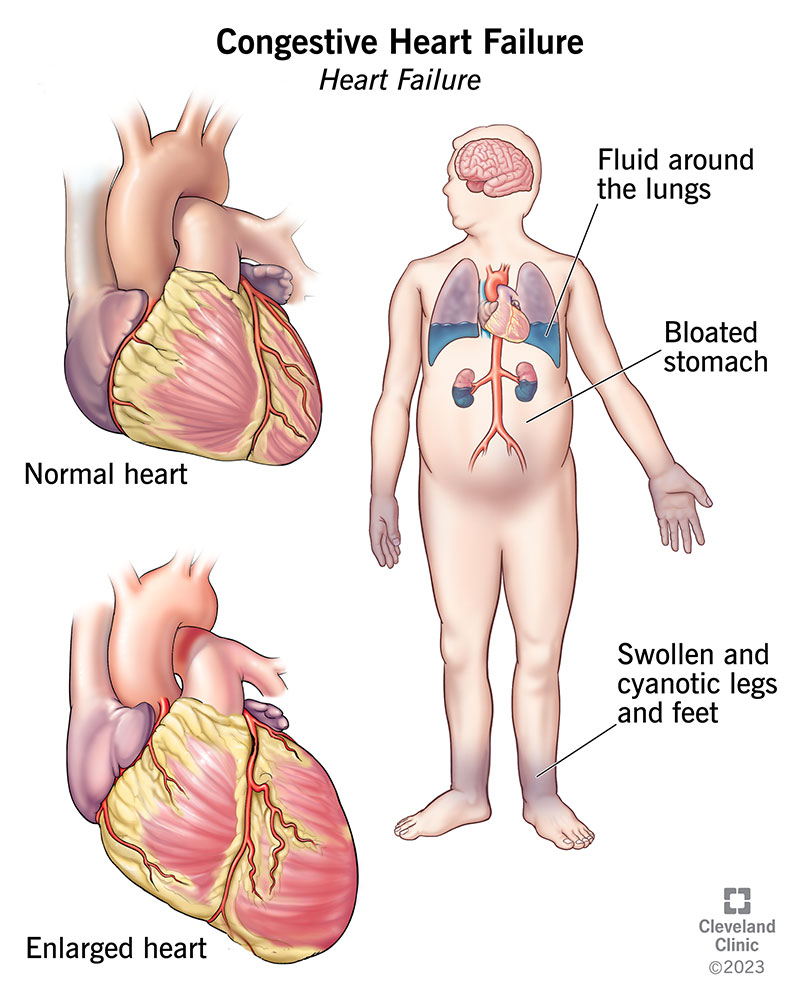
Understanding Diuretics
Diuretics help the body eliminate excess fluid by increasing urine output. They are often prescribed for:
- Congestive heart failure (CHF)
- Chronic kidney disease (CKD)
- Liver cirrhosis with ascites
- Hypertension (particularly with volume overload)
What Is Lasix?
Lasix, or furosemide, has been in clinical use since the 1960s. It’s known for its rapid onset (within 30–60 minutes orally) and potent diuretic action. Its short duration—roughly 6 hours—makes it ideal for quick fluid removal, but it often requires multiple doses per day.
Lasix is commonly used in emergency settings like acute pulmonary edema and for daily fluid control in CHF patients. However, it suffers from low oral bioavailability (around 50%), meaning the body doesn't absorb the entire dose effectively.
What Is Torsemide?
Torsemide (brand name Demadex) is a newer-generation loop diuretic. Though similar in mechanism to Lasix, Torsemide offers longer duration (12–16 hours) and higher bioavailability (up to 80%). This makes it more predictable and efficient in many clinical scenarios.
It’s especially useful in chronic heart failure management where consistent diuresis is critical. Studies suggest it may improve long-term outcomes better than Lasix—though not all physicians have fully transitioned to using it.
Onset and Duration: Speed vs. Endurance
Here's a comparison of key pharmacokinetics:
| Feature | Lasix (Furosemide) | Torsemide |
|---|---|---|
| Onset (oral) | 30–60 minutes | 60 minutes |
| Peak effect | 1–2 hours | 1–2 hours |
| Duration | 6–8 hours | 12–16 hours |
| Bioavailability | 40–60% | 80–100% |
In practical terms, Torsemide requires fewer daily doses and leads to more consistent fluid removal. This makes it attractive for outpatient use. 
Effectiveness in Heart Failure
Clinical trials have suggested that Torsemide may provide better symptom control and reduce hospitalizations in heart failure patients compared to Lasix. Its sustained action maintains lower central venous pressure and helps avoid the peaks and troughs of Lasix therapy.
A notable study, the TORIC trial, demonstrated that Torsemide improved functional class and reduced mortality more effectively than furosemide. As a result, many cardiologists are now reconsidering their diuretic protocols.
Electrolyte Impact and Safety Profile
Both drugs can cause:
- Low potassium (hypokalemia)
- Low magnesium (hypomagnesemia)
- Increased uric acid (risk of gout)
- Dehydration and low blood pressure
However, Torsemide appears to cause fewer fluctuations in electrolytes. It may also improve myocardial fibrosis and reduce sympathetic nervous system activation—two factors associated with better heart health.
Cost and Availability
Lasix is available in both generic and branded versions and is very inexpensive—often just a few cents per pill. Torsemide, while generic now, is still slightly more expensive. However, considering its once-daily dosing and lower hospitalization rates, it may prove cost-effective in the long term.
Insurance coverage typically includes both, but some formularies may prefer Lasix due to its lower price point.
Patient Experiences and Clinical Preferences
Many patients on Lasix complain of the "rush to the restroom" effect, followed by a quick fade in efficacy. Those switched to Torsemide often report more gradual, sustained relief with fewer bathroom emergencies. Physicians also prefer Torsemide for patients who miss doses or require consistent fluid control.
Nevertheless, Lasix still reigns in hospital settings due to familiarity and ease of intravenous administration in acute care.
Which One Should You Choose?
There’s no one-size-fits-all answer. Lasix remains a mainstay for acute settings and short-term use. Torsemide shines in chronic management, especially for heart failure patients needing stable diuresis.
Ultimately, the best choice depends on:
- Your specific condition (CHF, CKD, edema, etc.)
- Your response to each drug
- How well you tolerate the side effects
- Doctor and insurance preferences
So, who wins the duel? Torsemide may be the rising champion in the outpatient world, but Lasix still holds its crown in emergency rooms and ICUs. Either way, it’s a duel worth watching—and one your kidneys won’t forget.
